A Patient’s Guide to the Types of Vasectomy Reversal

Medical Director & Consultant Urologist
MBBS (Singapore), MRCS (Edin) FRCS-Urol (Glas), FAMS (Urol)
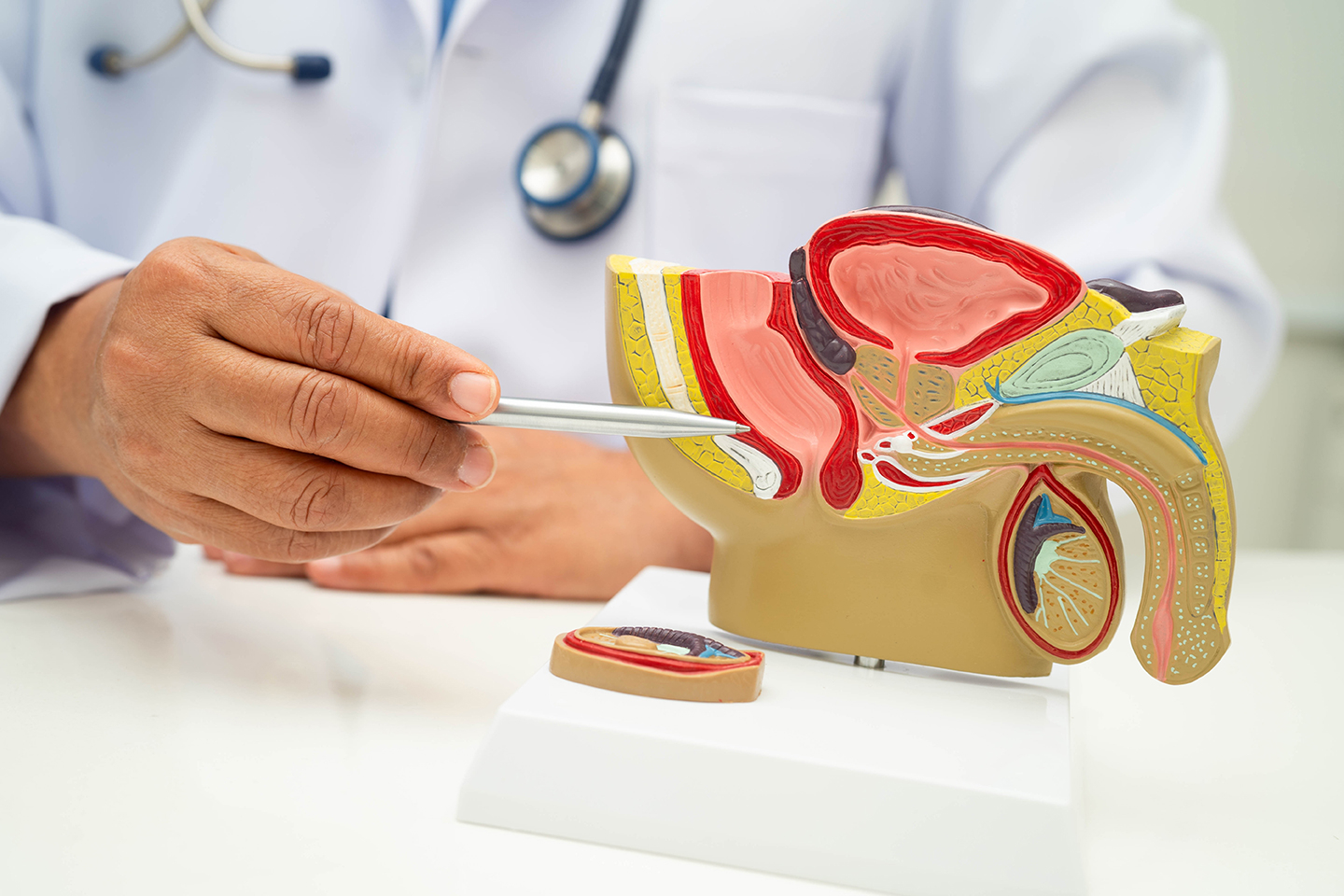
Decisions made at one stage of life may not always align with future circumstances. For some men, a vasectomy that once felt appropriate may later prompt reconsideration, particularly when plans around family change. In these situations, vasectomy reversal offers a potential path to restoring fertility.
Undergoing a vasectomy reversal is a significant step, and the procedure is not the same for every patient. In Singapore, vasovasostomy (VV) and vasoepididymostomy (VE) are the two surgical approaches used to reconnect the reproductive tract. Each differs in technique and complexity, and the choice between them depends on factors identified during surgery rather than personal preference alone.
What Is a Vasectomy Reversal?
A vasectomy prevents pregnancy by cutting or blocking the vas deferens: the tube that carries sperm from the testicles to the urethra. Vasectomy reversal, on the other hand, is a microsurgical procedure that aims to restore this pathway.
During the operation, the surgeon carefully assesses the reproductive tract to identify the most suitable point for reconnection. Blockages may occur not just at the original vasectomy site but also further upstream in the epididymis, which is a long, tightly coiled tube located at the back of each testicle. The choice of surgical approach depends on these findings, as the two techniques differ in how and where the reconnection is performed.
Understanding Vasovasostomy (VV)
Vasovasostomy reconnects the two separated ends of the vas deferens. This is the preferred method when fluid analysis during the operation suggests that the path leading from the testicle to the cut ends of the vas is clear of secondary obstruction.
During the surgery, the surgeon obtains a sample of fluid from the testicular end of the vas. The observation of whole sperm or sperm fragments in this fluid is a positive prognostic indicator, confirming that the upstream passage is open. When this is the case, the divided vasal ends are rejoined, thus restoring the original route for sperm movement.
Understanding Vasoepididymostomy (VE)
Vasoepididymostomy is employed when there is suspicion of an obstruction within the epididymis. This technique is designed to bypass the blocked segment by creating a new, direct connection between the vas deferens and a suitable tubule on the epididymis.
If fluid extracted from the vasal end is thick or appears non-existent, or if the epididymis appears tense, it may indicate a secondary blockage that has developed before the vasectomy site. In these situations, attaching the vas directly to the epididymal tubules allows sperm to bypass the blockage.
Differences Between VV and VE
The main difference lies in where the reconnection is made. Vasovasostomy reconnects the two cut ends of the vas deferens and is performed when there is no blockage beyond the vasectomy site, usually resulting in higher success rates. Vasoepididymostomy, on the other hand, connects the vas deferens directly to the epididymis and is required when a secondary blockage is present, which is more common after longer intervals since vasectomy. VE is more technically complex and generally has lower success rates, but it allows fertility to be restored when VV is not possible.
VV vs. VE: Factors to Consider
Although the final decision on which reversal technique to use is made during surgery, several patient-specific factors help guide expectations beforehand.
- Time Since Vasectomy: A longer interval between the original vasectomy and reversal increases the chance of secondary blockage in the epididymis, which may affect the type of reconnection required.
- Details of the Original Vasectomy: The amount of scarring and the length of vas deferens removed or sealed during the initial procedure can influence how easily the ends can be reconnected.
- Previous Scrotal Surgery or Trauma: Earlier injuries or surgical procedures in the scrotal area may alter tissue quality and affect the condition of the vas deferens and surrounding structures.
- Presence of a Sperm Granuloma: A sperm granuloma, which is a small lump that can form near the vasectomy site, is assessed during planning. Its presence may sometimes indicate pressure relief in the system and can influence surgical findings.
All these factors are taken into consideration to allow surgeons to anticipate the complexity of the procedure, even though the definitive approach is confirmed during the operation itself.
Recovery After Vasectomy Reversal
Recovery plays an important role in the overall success of a vasectomy reversal. Your surgeon will provide specific instructions and following them closely helps protect and support healing.
- Activity Adjustments: You will usually be advised to avoid strenuous exercise, heavy lifting and sexual activity for a period after surgery. These restrictions help prevent strain on the surgical site during the early healing phase.
- Support and Comfort: Wearing supportive underwear is commonly recommended to reduce swelling, provide comfort and minimise movement of the scrotum as it heals.
- Wound Care: Keeping the incision clean and dry is important. You may be advised to avoid soaking baths until cleared by your surgeon and to watch for signs of infection, such as redness or increasing pain.
- Follow-up Semen Analysis: Success is confirmed by the return of sperm to the ejaculate. This is usually checked through semen analysis several months after surgery, as it takes time for sperm production and transport to recover.
When to Seek Medical Attention After Vasectomy Reversal?
You should contact your doctor promptly if you notice any of the following signs, as they may indicate a complication that needs medical review:
- Increasing or severe pain that does not improve
- Fever or chills
- Discharge from the wound, such as pus or excessive fluid
- Persistent swelling or swelling that continues to increase
At Urology Practice, we are committed to providing advanced, personalised and affordable urological care. As a fellowship-trained consultant urologist with 19 years of medical experience, Dr Jonathan Teo will accurately assess your suitability, explain the differences between vasovasostomy and vasoepididymostomy and outline what to expect before, during and after surgery. Contact us for a personalised assessment and a discussion of the appropriate treatment options for you.

Our Urologist in Singapore
Dr Jonathan Teo
Medical Director & Consultant Urologist
Qualifications & Credentials:
- MBBS (Singapore) – National University of Singapore (NUS)
- MRCS (Edinburgh) – Royal College of Surgeons of Edinburgh
- FRCS-Urol (Glasgow) – Royal College of Physicians and Surgeons, Glasgow
- FAMS (Urology) – Fellow of the Academy of Medicine, Singapore
Dr Jonathan Teo is a fellowship-trained consultant urologist in Singapore with extensive expertise in men’s health, urological cancers, and minimally invasive treatments. He was formerly the Director of Andrology at Singapore General Hospital and an elected EXCO member of the Society of Men’s Health Singapore. Dr Teo specialises in erectile dysfunction, male subfertility, and advanced treatments for benign prostatic hyperplasia (BPH).
More About Dr Teo
